Introduction
le 16 mars dernier, sur Twitter, je publiais un fil sur les traitements par Inhibiteur de l’Enzyme de Conversion (IEC) (dont j’ai abordé la place dans l’insuffisance cardiaque à l’ouverture du blog dans 3 billets consécutifs leur découverte, leur indication et leur dose) et par Antagoniste des Récepteurs à l’Angiotensine II (ARA2).
Cette série de tweets faisait suite à des interrogations autour de la sécurité des ces deux classes thérapeutiques (IEC et ARA2), certains auteurs (dans le BMJ et dans le Lancet Respiratory Medicine notamment) laissant entendre qu’elles augmenteraient le risque de forme grave, et plusieurs twittos m’avaient interpellé pour avoir mon avis sur le sujet.
Suite à ce fil, j’ai décidé d’aller plus avant et d’en écrire un article complet, à soumettre à une revue à comité de lecture pour une publication. J’ai finalisé l’article avec Mathieu Rebeaud (@Damkyan_Omega) et nous l’avons soumis pour publication le 20 mars. Il a malheureusement été refusé. Dans les jours qui ont suivi, plusieurs articles sont parus sur le même sujet, dans le JAMA, l’European Heart Journal ou le NEJM (je n’ai pas encore lu ce dernier article), allant tous dans le même sens que mes conclusions initiales.
Afin que le travail ne soit pas perdu et fait pour rien, nous avons décidé de le publier ici tel qu’il a été soumis. Il est pour l’instant en anglais. Quand j’aurais un peu de temps, et en fonction de l’évolution des connaissances, je le traduirai et l’étofferai.
Bonne lecture
L’article
Following its outbreak in December 2019, Severe Acute Respiratory Syndrome CoronaVirus 2 (SARS- CoV-2) spread to the whole world. Many efforts are made to identify risk factors predisposing to a severe issue. In the larger published cohort of SARS-CoV-2, history of hypertension is more prevalent in patient with severe disease (1). Nevertheless, these data are not adjusted for age, and hypertension is a very common finding in older patients.
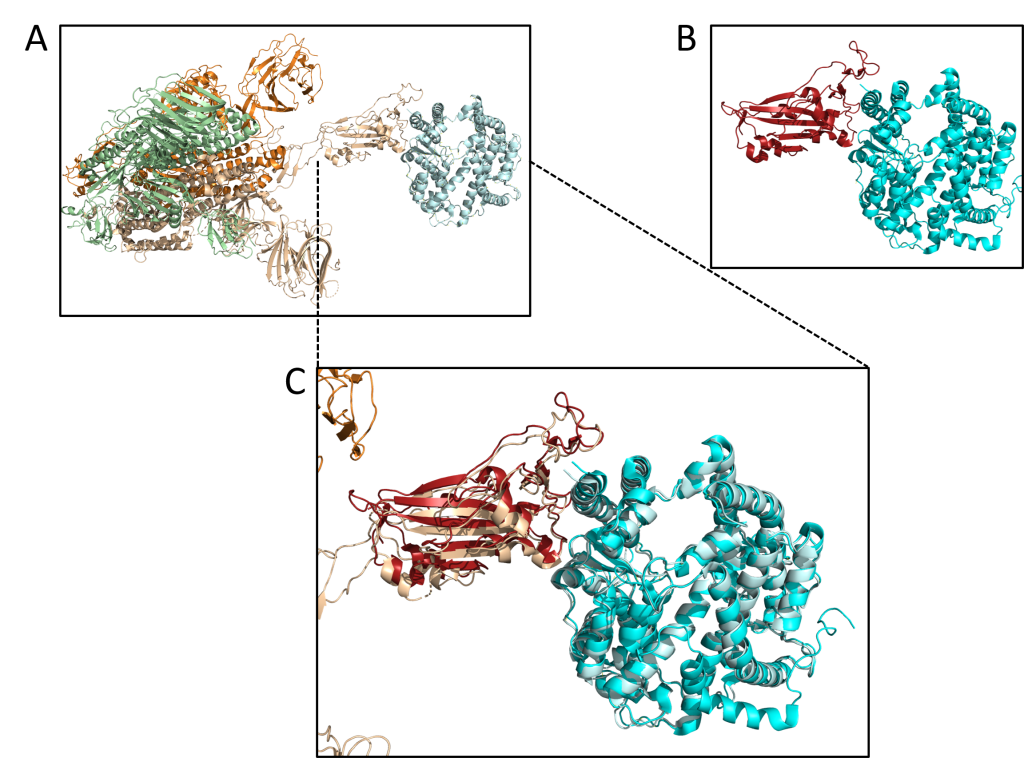
Publications:
PDB ID: 6CS2 ; Kirchdoerfer, R.N., Wang, N., Pallesen, J., Wrapp, D., Turner, H.L., Cottrell, C.A., Corbett, K.S., Graham, B.S., McLellan, J.S., Ward, A.B. (2018) Sci Rep 8: 15701-15701
PDB ID: 6M0J ; Wang, X., Lan, J., Ge, J., Yu, J., Shan, S., (2020) Crystal structure of 2019-nCoV spike receptor-binding domain bound with ACE2 DOI:10.2210/pdb6M0J/pdb
Like SARS-CoV, SARS-CoV-2 enters into human cells after the receptor-binding domain of its S (Spike) protein binds with Angiotensin-Converting Enzyme 2 (ACE-2), an enzyme located in particular on lung alveolar epithelial cells and cardiomyocytes (2–4) (fig 1). ACE-2 is homologous to Angiotensin-Converting Enzyme (ACE) but is not inhibited by ACE inhibitors (ACEi) (3,5). ACE cleaves angiotensin I to generate angiotensin II (ANGII) which binds to and activates Angiotensin Type 1 Receptor (AT1R), elevating blood pressure (5). ACE2 downregulates AT1R and inactivates ANGII by converting it to angiotensin 1-7 which has a vasodilator effect (5). Thus, ACE2 negatively modulates renin-angiotensin system (3,5). In rats, ACE2 deficiency worsens hypertension when ANGII is in excess (3,6). In human, gene expression and/or ACE2 activity is lower in hypertensive patients than in normotensive ones (6). In the heart, ACE2 loss leads to a decrease in myocardial function in rodents, likely mediated by ANGII-induced oxidative stress and inflammation through AT1R (3). This decrease is corrected by AT1R blockers (ARB) or ACEi (3).
ANGII decreases ACE2 expression through an AT1R-dependent mechanism and ACEi/ARB upregulate ACE2 expression (3,5,6). Patients treated with ACEi/ARB could have a higher level of ACE2, providing more potent binding site to COVID-19 S protein. Nevertheless, in the absence of excess ANGII (either by reduction of ANGII synthesis by ACEi or by AT1R blockade thanks to ARB) AT1R interacts with ACE2 (5). This interaction could reduce affinity of COVID S protein to ACE2 and reduce viral entry despite a larger number of ACE2 (5).
In both heart and lung binding of the SARS-CoV to ACE2 leads to loss of ACE2 by ACE2 internalization with the virus and ACE2 shedding (4). Lower availability of ACE2 results to a lower rate of ANG2 degradation (7). Excess ANG2 binds to AT1R and increases pulmonary vascular permeability, enhancing lung injury (7). Thus, decreased ACE2 expression promotes lung injury and ARB prevent it by limiting ANG2 binding to AT1R (3,7). This hypothesis is supported in vivo by the increased frequency of severe ARDS in patient with higher level of ACE determined by genetic predisposition, leading to higher level of ANGII (8). As in lungs, ANGII probably contributes to the deleterious effect of SARS-CoV on the heart, even if myocardial dysfunction can also be influenced by a strong immune response (4). Inflammatory signals are likely to suppress ACE2 transcription and could increase the ANGII excess (3). To summarize, less cellular ACE2 leads to more AT1R activation and more severe injuries. To the contrary, the greater the number of ACE2 on the cell membrane, the lesser the injury, thanks to a reduced AT1R activation. This later condition is the one provoked by ACEi/ARB treatment. ARB supplementary inhibits AT1R and limits injury induced by its overstimulation.
Because ACEi/ARB upregulates ACE2, several authors hypothesized a potential deleterious effect of these treatment in SARS-CoV-2 infection course (9,10). But, even if ACEi/ARB increase ACE2 level, more ACE2 might be better than worse. It is unclear whether continuing or stopping ACEi/ARB is a good option in COVID19 infection, or if treatment with ACEi/ARB is beneficial or harmful on virus-mediated injuries, because clinical data are lacking. Some clinical trials are ongoing to analyze beneficial effect of LOSARTAN in COVID-19 (NCT04311177 and NCT04312009).
To sum, ACEi/ARB mediated ACE2 increase is not obviously deleterious and can even be protective. Only well conducted trial will provide valuable answer to this question. To date, ACEi/ARB must not be stopped. Moreover, if the decreased amount of cellular ACE2 in hypertension is really linked to a worse prognosis, hypothesis can be made that non-ACEi/ARB drugs (betablockers, calcium channel blockers, diuretics) are more likely to increase the risk of deleterious course than ACEi/ARB which increase ACE2 and provide a theoretical protection.
References
1. Guan W, Ni Z, Hu Y, Liang W, Ou C, He J, et al. Clinical Characteristics of Coronavirus Disease 2019 in China. N Engl J Med. 28 févr 2020;0(0):null.
2. Lu R, Zhao X, Li J, Niu P, Yang B, Wu H, et al. Genomic characterisation and epidemiology of 2019 novel coronavirus: implications for virus origins and receptor binding. The Lancet. 22 févr 2020;395(10224):565‑74.
3. Kuba K, Imai Y, Ohto-Nakanishi T, Penninger JM. Trilogy of ACE2: A peptidase in the renin–angiotensin system, a SARS receptor, and a partner for amino acid transporters. Pharmacol Ther. 1 oct 2010;128(1):119‑28.
4. Oudit GY, Kassiri Z, Jiang C, Liu PP, Poutanen SM, Penninger JM, et al. SARS-coronavirus modulation of myocardial ACE2 expression and inflammation in patients with SARS. Eur J Clin Invest. 2009;39(7):618‑25.
5. Deshotels Matthew R., Xia Huijing, Sriramula Srinivas, Lazartigues Eric, Filipeanu Catalin M. Angiotensin II Mediates Angiotensin Converting Enzyme Type 2 Internalization and Degradation Through an Angiotensin II Type I Receptor–Dependent Mechanism. Hypertension. 1 déc 2014;64(6):1368‑75.
6. Soler MJ, Wysocki J, Batlle D. ACE2 alterations in kidney disease. Nephrol Dial Transplant. 1 nov 2013;28(11):2687‑97.
7. Imai Y, Kuba K, Rao S, Huan Y, Guo F, Guan B, et al. Angiotensin-converting enzyme 2 protects from severe acute lung failure. Nature. juill 2005;436(7047):112‑6.
8. Itoyama S, Keicho N, Quy T, Phi NC, Long HT, Ha LD, et al. ACE1 polymorphism and progression of SARS. Biochem Biophys Res Commun. 22 oct 2004;323(3):1124‑9.
9. Sommerstein, Rami, Gräni, Christophe. Re: Preventing a covid-19 pandemic: ACE inhibitors as a potential risk factor for fatal Covid-19. BMJ. 14 mars 2020;368:m810.
10. Fang L, Karakiulakis G, Roth M. Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection? Lancet Respir Med [Internet]. 11 mars 2020 [cité 15 mars 2020];0(0). Disponible sur: https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(20)30116-8/abstract
